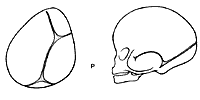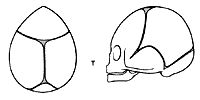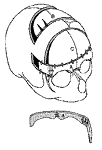of Main Conditions Managed
Visible scars are avoided as far as possible. The main approach to the craniofacial skeleton is made through the hairy scalp. A long incision from ear to ear is performed, with a zigzag in the temporal region. This type of incision enables good exposure and usually remains practically invisible after closure.
The hair is not shaved. An additional incision is sometimes performed at the eyelid level, with no scar if inside the eyelid, or a nearly invisible scar if in the skin of the eyelid. Sometimes, an opening is also made in the mucosa of the mouth, at the inner side of the lip..
In some severe cases of medial cleft and hypertelorism, an incision on the nose, to remove an excess of skin or repair a distortion, is necessary. Also, very exceptionally, the forehead, eyelids or cheeks have to be approached by direct incisions.
Craniosynostosis – Frontocranial Remodeling
The deformed skull will be corrected by mobilizing the distorted part or parts and by maintaining them in normal position by adapted fixation.
The craniosynostosis are operated usually during the first year of life. At this age, the reossification of bone defects is fast, and one can leave, after repositioning, open gaps that will close rapidly.
A different procedure is performed for each type of craniosynostosis
Most common craniosynostosis
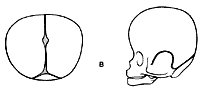
Brachycephaly (recessed and often vertical forehead).
An advancement of the supraorbital ridge is performed and the forehead advanced accordingly.
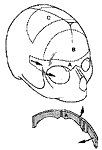
Correction of a brachycephaly. Supra orbital barr is advanced 10 to 20 mm.
Fixations are made at the facial and frontal level.
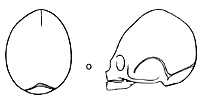
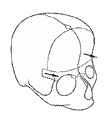
Oxycephaly (backward tilted forehead with pointed head).
This is usually a late-appearing deformity, between 3 and 5 years of age. Correction is obtained by rocking and advancement of the supraorbital ridge and frontal correction.
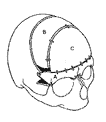
Correction of an oxycephaly.Removal of supra orbital barr A which is then advanced and rocked.Removal of flattened forehead B which is exchanged the C of good curvature.
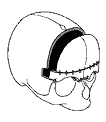
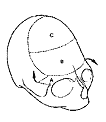
Plagiocephaly (asymmetry of the forehead, orbits and nose).
A bilateral correction is performed, advancing the recessed side and reconstructing a one-piece forehead in normal position.
Correction of a right plagiocephaly.Removal of supra orbital barr A which is straightened. Removal of distorted forehead B which is replaced by a suitable piece taken from the cranial vault.
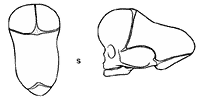
Scaphocephaly (elongation and narrowing of the skull).
When detected early, a simple operation of enlarging the medial restricted part of the skull is sufficient. When discovered later, or in some severe cases, a remodelling of the frontal and posterior part of the skull has to be performed as well.
Trigonocephaly (triangular forehead with a midline crest).
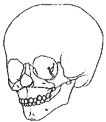
The frontal part of the skull is corrected by straightening the supraorbital ridge and reconstructing a normal frontal bone.
Facial Advancement
A retruded midfacial mass is observed in faciocraniosynostosis. The upper teeth are recessed, the nose is small, the eyes are protruding.
The correction of this anomaly is obtained by an advancement, after an osteotomy performed to allow to mobilize the retruded parts.
Most frequently the advancement is a Le Fort III osteotomy, advancing the nose, the malar bones, the upper maxilla.
Sometimes a Le Fort II is performed, leaving the malar bones in place.
A Le Fort I advances only the upper maxilla, along with the upper teeth.
Distraction is used in selected cases to place the advance skeleton in the desired position. An orthodontic preparation and follow-up is very important (cf chapter « Distraction »).
Hypertelorism Correction
The distance between the orbits must be reduced by resecting part of the enlarged nose.
The orbits are brought together after circumferential osteotomies have been performed..
Sometimes, a medial vertical slit is made between the incisor teeth. It will allow for enlarging the upper part of the mouth.
The excess bone in the middle is removed and the two hemi-faces
are brought together enlarging the upper Dental arch….
Orbital asymmetry, Orbital dystopia
According to the case, one will mobilize one orbit, usually as a box, « en bloc », to bring it to the desired position and level. Sometimes one mobilizes differently the two orbits if an hypertelorism, an enlargement of the interorbital distance, is associated.
Distraction Osteogenesis : Faciocraniosynostosis treatment
Surgical treatment of faciocraniosynostosis involves complex techniques which must address two issues:
Prevention of cerebral damage secondary to craniosynostosis (most commonly bi-coronal or multiple).
Optimal morphological correction of facial retrusion and resultant exorbitism (which threatens vision when severe) and of the upper airways to improve respiratory function.
The conventional approach to the cranium involves augmentation of its volume with a fronto-orbital advancement, best performed before one year of age. This cranio-orbital intervention corrects the problems associated with craniosynostosis in one single procedure in the vast majority of cases. Cerebral growth is almost complete by three years of age and the risks to the brain are minimal after this time.
For those in whom there is facial retrusion, correction is performed at a variable age depending on the severity of the deformity and its aesthetic and functional consequences. Facial growth is complete at around 16-18 years and operative treatment is therefore performed at this age to correct facial malformations definitively in one procedure. Whereas this strategy is applicable for minimal deformities, it is not possible to delay facial correction in those children who display more severe malformation, without the risk of major psychological sequelae. In such cases it is possible to operate sooner, accepting that since the genetic growth disturbance will remain, further surgery will be required in due course. Generally, the magnitude of the requisite interventions decreases as the years pass.
Two stage strategy:
Distraction osteogenesis (distraction being the reverse of contraction) is an a surgical option which allows a gradual separation of bone over time. This innovative approach was initially applied to the mandible (McCarthy in New York, Molina in Mexico, Diner in Paris), and was subsequently applied to the bones of the craniofacial skeleton.
Since 1995, we have applied the techniques of distraction osteogenesis to Le Fort III facial advancements. This has allowed early correction of facial retrusion in younger children requesting treatment or requiring treatment for respiratory compromise (snoring, sleep apnoea or hypoxaemia in more severe cases). This approach therefore requires two principal interventions (cranial surgery and facial distraction surgery) followed by minor facial procedures. This two stage approach is still the classical management, despite the fact that distraction techniques allow further refinements in the treatment of even younger children:
A one stage surgical strategy has existed for some time, but was almost abandoned because of the risks involved; fronto-facial monobloc advancement (1978, Ortiz-Monasterio) allows simultaneous correction of the various deformities of the forehead and the face. But this procedure which is technically complex, results in two inevitable consequences which are associated with not insignificant danger: These are, a retro-frontal dead space and a communication between this space and the upper part of the nasal airways as a result of the anterior cranial osteotomies. Major complications (meningitis, frontal bone necrosis) can ensue, particularly when the anterior cerebral re-expansion is not rapid enough, which is the case in adults or older children. These risks have resulted in the majority of teams drastically reducing the indications for classical Monobloc advancements, despite certain technical modifications having been proposed in order to attempt to reduce these risks; specifically ensuring a watertight repair of the anterior fossa floor and filling the deadspace with a flap or split forehead.
The use of distraction osteogenesis for fronto-facial monobloc advancement has been performed since the year 2000 in our unit. We have operated on more than 40 cases with this technique with good results, especially with regard to the improvement of respiratory function and the correction of exorbitism. The morbidity in the monobloc procedure can be significantly reduced as a result of distraction. We have developed our protocol using two pairs of external distractors which seem to improve the effectiveness of the procedure, while also decreasing its morbidity. The progressive experience gained has resulted in gradual changes in the surgical technique as well as the distraction protocol.
Surgical technique and distractors:
The surgical technique used, is a fronto-facial monobloc osteotomy, this is performed without removal of the frontal bone. The bilateral pterygo-maxillary disjunction aswell as the division of midline structures are performed systematically allowing operative mobilisation of the complete fronto-facial assembly.
The distractors used are prototypes manufactured by Martin-Medezin with cylinders controlled by a percutaneous flexible device. Two types of distractors are necessary; frontocranial distractors used in the supra-orbital region and temporo-malar distractors with a rotatory axis (modifations of the distractors originally produced by MicroFrance-Xomed) and positioned behind the zygomas. The control mechanism of the lower distractors are exteriorised posteriorly in all patients. The superior distractors are also exteriorised posteriorly. In one of our patients however, the superior distractor was exteriorised anteriorly through the eyebrow in an approach we no longer recommend. The screws used to fix the distractors in place are resorbable (Bionix, diameter 2mm or Champy 2mm). When fronto-zygomatic support is required, resorbable or metallic miniplates are used. In one of our patients undergoing secondary surgery a reconstruction of the bandeau had to be undertaken and a transfacial pin (Staca, 2mm) as described by Pellerin was connected to the anterior extremity of the two temporo-malar retractors to re-inforce the assembly and maintain control of the facial bipartition.
Distraction protocol:
The distraction protocol was classical for the first 15 patients, with a daily advancement of around 1mm in each of the first four patients. The start of distraction was deferred to the 7th or 8th day. In the immediate post-operative period, no major infective episodes were noted, although a pyrexia of 37.5 – 38 ˚C was present in all patients over the first few days.
The distraction was achieved with 0.9mm daily advancement of the frontal distractors (3 turns of 3mm each) and with 1mm daily advancemt of the temporal distractors (2 turns of 0.5mm). Distraction was continued to the maximal extent (15mm) in the frontal distrators, which required some 14 to 17 days, depending on the initial position of the cylinders. The duration of temporo-zygomatic distraction was longer as the distractors do not have a limiting abutment, and was around 20 – 28 days, until class 1 occlusion was achieved. By the end of the distraction period, the control mechanisms of the distractors were sectioned flush with the skin and an arrangement made to remove the distractors at least 3 months later, in the first 6 patients. This consolidation period has progressively increased to 9 months with subsequent patients, in order to decrease the degree of bony resorbtion and fronto facial retraction seen in distractors removed too early.